Harvey: An Educational Tool for NYMC for More Than 20 Years
The Cardiology Patient Simulator Has Taught NYMC Students Since 1998
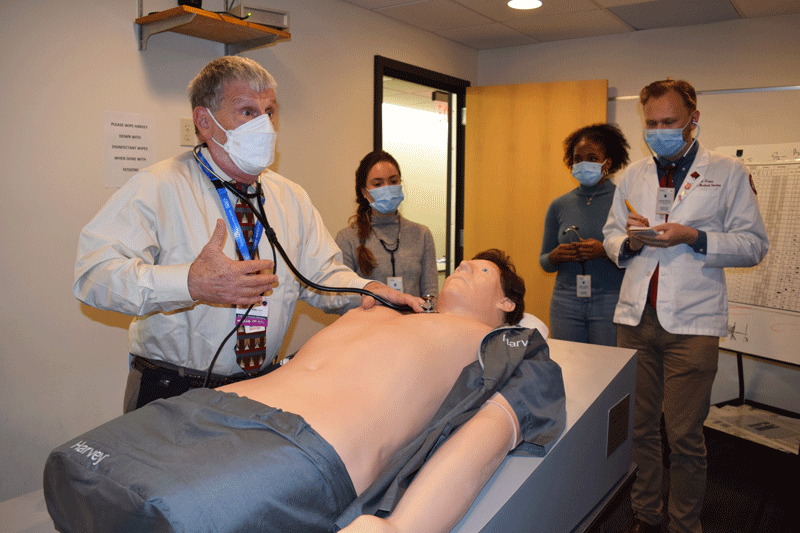
Students and faculty have got to know Harvey on a first name basis ever since the shaggy-haired manikin's arrival on campus in 1998. Harvey, a Cardiopulmonary Patient Simulator, helps learners to master their clinical skills related to identifying the nuances of cardiopulmonary sounds, implementing diagnostic interventions and developing therapeutic treatment plans. With a touch of a button, the life-sized Harvey manikins can be programmed to simulate nearly 50 clinical findings found in children and adults. Harvey takes students outside of a traditional classroom setting by providing hands on training utilizing specialized headsets, corresponding to a technologically advanced stethoscope, related to recognizing variations in blood pressure, pulses, heart sounds, murmurs and breath sounds.
When Harvey was introduced to the school, the manikin was used by the School of Medicine (SOM) second-year medical students in a back room of the Phillip Capozzi, M.D., Library. Now, the two updated Harveys purchased in 2018, located in the Clinical Skills and Simulation Center, are also used in various SOM clerkship assessments, School of Health Sciences and Practice’s Department of Physical Therapy, Touro College of Dental Medicine, Westchester Medical Center residency programs and the Envision High School Program for Health Sciences to train students on cardiac and pulmonary pathologies, the functionality and response of the heart and lungs and cardiopulmonary emergencies. The Harveys are incorporated early in the curriculum and are used not only as a tool of training, but as a key piece of lifelong learning.
Like any other technology, Harvey keeps getting better with age. The College’s first Harvey could be programmed to replicate 27 cardiac conditions, including two normal and 25 cardiovascular diseases, through replicated blood pressure and venous, arterial and precordial pulses. Additional computer programs allow students to further evaluate Harvey by providing clinical findings, laboratory data and therapeutic inventions based actual patients. Now, the manikin can make dozens of more sounds that are clearer than before. The newest model of Harvey also comes with additional learning tools, including online modules, quizzes and other enhancements to add to the teaching experience.
“The more varied learning opportunities educators can provide students with creates more chances for repetition and learning as well as ensuring all the different learning styles of students get met,” said Kristina M. Welsome, PT, D.P.T., M.S., OCS, MTC, CFMT, NBC-HWC, assistant professor of clinical physical therapy. “The novelty of Harvey makes learning fun.”
“You can go to YouTube and hear pretty much every cardiopulmonary sound that you want, but that's not the same as being in a room with a stethoscope and a body that looks realistic and seeing the main artery moving, feeling that the vibration of it,” said Katharine Yamulla, M.A., CHSE, senior director of competency-based assessment and clinical skills education and director of the Clinical Skills and Simulation Center. “There's that reality of touching a patient that creates a vital sense memory for future recognition of cardiopulmonary sounds.”
The first Harvey was displayed in 1968 at the American Heart Association Scientific Sessions. The late Michael S. Gordon, M.D., founder and director emeritus of the Michael S. Gordon Center for Research in Medical Education at University of Miami Miller School of Medicine, along with cardiologists, educators and engineers developed Harvey and its multimedia elements after decades of creating the educational curricula and tutorials. The manikin was named after W. Proctor Harvey, M.D., a Georgetown University cardiologist and mentor to Dr. Gordon. Harvey is used in nearly 700 medical centers worldwide.
