Medical Students Receive POCUS Training
With the advancement of the technology used in ultrasounds, smaller, portable devices are becoming more widely available and used in more applications in the medical field.
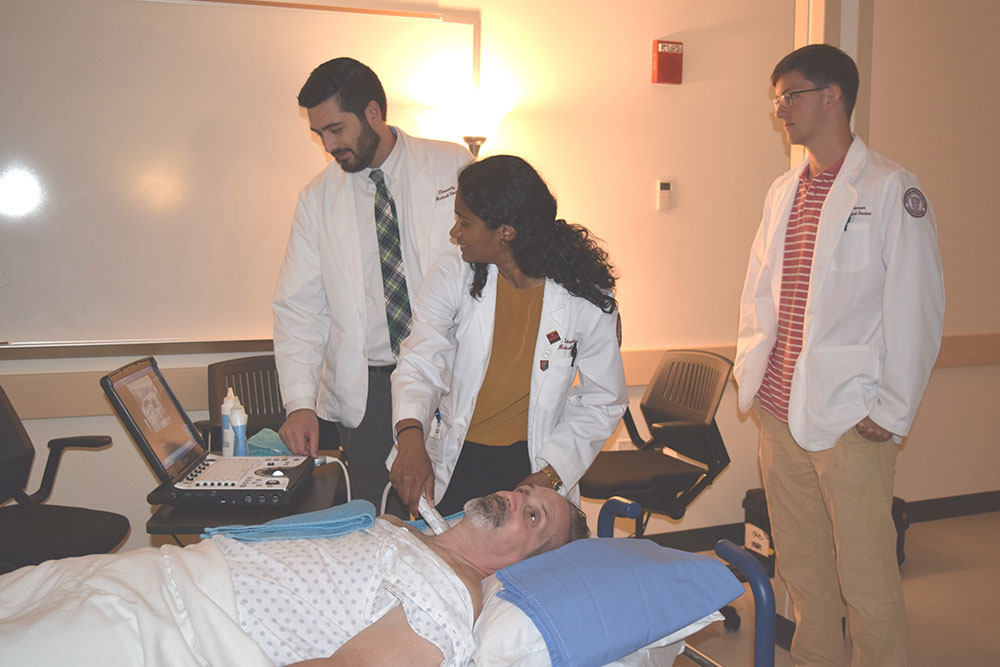
Point-of-care ultrasound (POCUS) allows trained medical professionals to use ultrasound to diagnose problems wherever a patient is being treated, whether it be in a modern hospital, an ambulance or remote foreign location. A new training program, Introduction to Point-of-Care Ultrasound, was conducted for 12 second-year medical students participating in the School of Medicine (SOM) summer fellowship program in emergency medicine on July 16 at the Clinical Skills and Simulation Center.
Students had the opportunity to perform ultrasounds on standardized patients with physician mentors. The training was sponsored by the Center for Disaster Medicine with funding through the Center of Excellence in Precision Responses to Bioterrorism and Disasters and support by Fujifilm/Sonosite and GE Healthcare who provided the new state-of-the-art ultrasound machines for the training.
A similar pilot training, held last year as part of a fourth-year elective, received high praise from students who advocated for the introduction of this training earlier in their undergraduate medical education.
“Having ultrasound training early on in our medical education definitely puts us at an advantage when we are out in a clinical setting, especially in the emergency department where ultrasound machines are accessible. Not only can we watch ultrasounds with a better understanding now, but we can use them on patients with a high degree of confidence after having practiced on standardized patients during our training,” said Jeanette Freeman, SOM Class of 2022. “I feel like I have an edge since I can help expedite treatment through the use of this tool.”
“Many medical students aren’t afforded the opportunity to learn about ultrasound during medical school. Instead they have to learn on the job. It was a great experience to learn the science behind ultrasounds in the morning and then get the chance to use multiple ultrasound machines in the afternoon,” explained Juliet Jacobson, SOM Class of 2022. “We learned how to use the machines for the musculoskeletal system to see fractures or torn tendons, for the abdomen to do a FAST exam and look for trauma to abdominal organs, for the thorax to look at the heart, and for venipuncture to properly insert peripheral and central lines. It not only was really interesting and helpful, but it was also quite relevant since I showed up to the emergency room at Metropolitan Hospital the next day and was asked to help with a FAST exam and examine a patient’s gallbladder with the ultrasound.”
“We are pleased to be able to offer this valuable educational experience to our summer students as they enter their second-year of medical school and can begin to integrate the fundamentals of gross anatomy with the use of diagnostic imaging to help determine where pathology may exist,” said David Markenson, M.D., M.B.A., director and medical director of the Center for Disaster Medicine. “Providing clinical awareness and training in the importance of ultrasound early on in the curriculum gives our medical students additional skills and abilities and is really cutting edge. It’s exciting to incorporate this emerging topic into our medical education at NYMC.”
